Plantar Fasciitis: Causes, Symptoms, Effects, Prevention
and Homeopathic Remedies for Plantar Fasciitis
Introduction
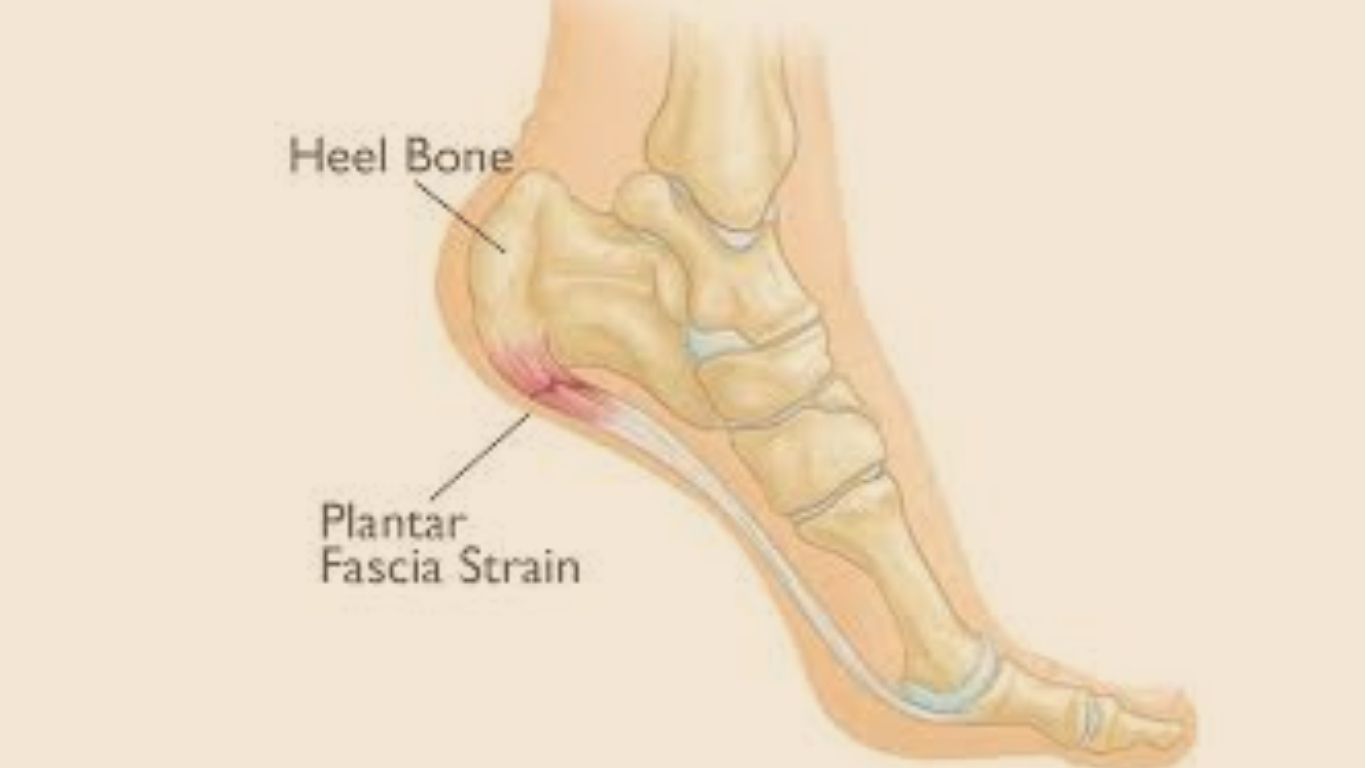
Plantar fasciitis is one of the most common causes of heel pain, affecting millions of people worldwide. Despite its prevalence, it remains a condition that is often misunderstood, leading to frustration for those who suffer from its persistent discomfort. The condition derives its name from the plantar fascia, a thick, web-like ligament that connects your heel bone to your toes, supporting the arch of your foot. When this structure becomes overstretched, overworked, or inflamed, it results in the stabbing pain that characterizes plantar fasciitis. This article aims to provide a thorough, human-centered exploration of the condition—delving into its symptoms, underlying causes, far-reaching effects, practical prevention strategies, and the role of homeopathic treatment as a complementary approach.
Recognizing the Symptoms
The hallmark symptom of plantar fasciitis is a sharp, stabbing pain in the bottom of the heel. However, the way this pain manifests can be quite specific and telling. Most people describe the discomfort as being most intense with the first few steps after waking up in the morning. After a night of rest, the plantar fascia has had time to contract and tighten; suddenly bearing weight on it causes micro-tears to stretch abruptly, leading to that characteristic jolt of pain.
As the day progresses and the tissues warm up, the pain often subsides to a dull ache, only to return after prolonged periods of standing, walking, or after sitting for an extended time. For instance, someone might feel fine after a morning walk, but after sitting at a desk for an hour, standing up again triggers a familiar twinge. This pattern is known as “post-static dyskinesia,” a term used to describe pain that occurs after periods of inactivity.
Other symptoms can include a gradual onset of pain over time rather than a sudden injury, mild swelling in the heel area, and a feeling of tightness or stiffness in the arch of the foot. In some cases, the pain may radiate outward, though it typically remains centered near the heel bone. It is important to note that while the pain can be severe, it is rarely accompanied by redness, significant heat, or visible deformity—if these are present, other conditions such as infection, stress fracture, or arthritis may be at play, warranting immediate medical attention.
Exploring the Causes
Plantar fasciitis is rarely the result of a single incident. Instead, it is typically a cumulative stress injury, meaning it develops over time due to repetitive strain and a combination of contributing factors. At its core, the condition arises when the plantar fascia is subjected to more tension than it can comfortably handle.
One of the primary causes is biomechanical imbalance. People with flat feet (overpronation) have a plantar fascia that is constantly stretched beyond its normal length, while those with unusually high arches (supination) place excessive tension on the fascia due to a lack of shock absorption. In both cases, the fascia becomes a compensatory structure, bearing loads it was not designed to carry repeatedly.
Improper footwear is another significant contributor. Shoes with inadequate arch support, thin soles, or poor cushioning fail to protect the foot from the impact of walking on hard surfaces. Similarly, wearing high heels regularly can shorten the Achilles tendon and calf muscles over time; when flat shoes are worn, the sudden change in angle places sudden, excessive strain on the plantar fascia.
Lifestyle and occupational factors play a crucial role as well. Individuals whose jobs require long hours of standing or walking on concrete floors—such as factory workers, teachers, retail staff, and healthcare professionals—are at heightened risk. Obesity is a major risk factor, as excess body weight multiplies the pressure exerted on the plantar fascia with every step. Sudden increases in physical activity, such as starting a new running regimen or significantly increasing walking distance without proper conditioning, can also trigger the condition.
Age is another element; plantar fasciitis is most common between the ages of 40 and 60, though it can affect younger individuals who are very active. Tight calf muscles and a tight Achilles tendon are often underlying culprits, as they limit ankle flexibility and force the plantar fascia to absorb more shock than it otherwise would.
The Effects Beyond Physical Pain
While plantar fasciitis is classified as a musculoskeletal condition, its effects often extend far beyond physical discomfort. Chronic heel pain can profoundly impact a person’s quality of life, influencing their mobility, emotional well-being, and even their social interactions.
On a physical level, the body is remarkably adaptive, and when someone alters their gait to avoid heel pain, they develop a limp or begin to shift weight to the opposite foot. This compensation can lead to secondary issues such as knee pain, hip pain, and lower back strain. Over time, these compensatory patterns can create a cascade of musculoskeletal problems that outlast the original foot condition.
The psychological toll is equally significant. Living with persistent pain that recurs with every step can lead to frustration, anxiety, and even depression. Many people find themselves avoiding activities they once enjoyed—whether it’s a daily walk, playing with children or grandchildren, or participating in a favorite sport. This withdrawal can lead to feelings of isolation and a sense of losing one’s identity, particularly for those who pride themselves on being active.
Sleep disturbances are common, as the pain can interrupt rest, especially when getting up during the night. The cumulative effect of poor sleep, chronic pain, and reduced activity can contribute to weight gain, which in turn worsens the original condition, creating a vicious cycle that becomes increasingly difficult to break.
From a socioeconomic perspective, plantar fasciitis is a leading cause of missed workdays and reduced productivity. For individuals in physically demanding jobs, the inability to perform tasks without pain can threaten their livelihood. Even for those in sedentary occupations, the discomfort of commuting or moving around the office can become a daily struggle.
Prevention Strategies
Preventing plantar fasciitis is largely about respecting the mechanics of the foot and making consistent, mindful choices. Because the condition is often the result of accumulated stress, prevention focuses on reducing that stress before it reaches a critical threshold.
Footwear is the first line of defense. Shoes should provide proper arch support, adequate cushioning, and a slightly raised heel to reduce tension on the Achilles tendon. For those who are prone to foot issues, rotating between different pairs of shoes can prevent repetitive pressure on the same areas. It is also advisable to avoid walking barefoot on hard surfaces for extended periods, as this offers no support to the arch.
Stretching and strengthening exercises are perhaps the most effective preventive measures. Regular stretching of the calf muscles and the plantar fascia itself can maintain flexibility and reduce tension. A simple yet powerful stretch involves pulling the toes back toward the shin to lengthen the arch, especially before taking the first steps in the morning. Strengthening the intrinsic muscles of the foot—through exercises like toe curls, marble pickups, or using a resistance band—can provide better dynamic support to the arch.
Weight management is another critical component. Even modest weight loss can significantly reduce the load on the plantar fascia with each step. For every pound of body weight, the force exerted on the feet with walking is approximately three to four times that amount. Thus, losing ten pounds can translate to a reduction of thirty to forty pounds of pressure per step.
For athletes and active individuals, a gradual approach to training is essential. Increasing mileage, intensity, or duration too quickly is a common trigger. Incorporating cross-training activities that are low-impact, such as swimming or cycling, can maintain cardiovascular fitness while giving the feet a rest. Proper warm-up and cool-down routines, including stretching, should never be skipped.
Those in occupations that require prolonged standing should consider using anti-fatigue mats, taking regular sitting breaks, and wearing supportive, occupation-appropriate footwear. Even small changes, such as avoiding standing in one position for too long and shifting weight frequently, can make a meaningful difference.
Homeopathic Treatment: A Complementary Approach
Homeopathy offers a unique perspective on plantar fasciitis, treating it not merely as a localized inflammation but as a manifestation of the individual’s overall susceptibility. In homeopathic practice, the goal is to stimulate the body’s self-healing mechanisms by using highly diluted substances that, in larger doses, might produce symptoms similar to those being treated. It is important to note that homeopathy is a complementary therapy, and individuals should consult with a qualified practitioner for personalized treatment. However, several homeopathic remedies are commonly associated with relief from plantar fasciitis symptoms, based on the principle of “like cures like” and the totality of the individual’s symptoms.
Ruta graveolens is often considered one of the primary remedies for plantar fasciitis, particularly when the pain involves the periosteum (the membrane covering the bone) and tendons. It is indicated when there is a feeling of bruising, soreness, and lameness, especially after overuse or injury. Individuals who benefit from Ruta often experience aggravation from cold and damp weather and find that the pain improves with continued gentle motion but returns with rest.
Rhus toxicodendron is another frequently used remedy, particularly when the pain is characterized by stiffness and a need to keep moving. The classic indication for Rhus tox is pain that is worse upon initial movement, improves with continued motion, and then returns after resting. This pattern closely mirrors the morning pain of plantar fasciitis. People who respond well to this remedy often feel restless and find that heat, such as warm baths or compresses, provides relief.
Calcarea fluorica is indicated when there is a tendency toward hard, nodular swelling, varicose veins, or a general weakness of the ligaments. It is often considered for chronic cases where the plantar fascia has lost its elasticity, and there is a sensation of tearing or straining in the tissues. This remedy may be particularly suited to individuals with a history of joint issues or those who feel that their tissues are “loose” and unsupportive.
Arnica montana is widely known for its use in trauma and overuse injuries. In the context of plantar fasciitis, it can be helpful when the condition is triggered by a specific physical strain—such as a long hike or a sudden increase in exercise—and when the feet feel bruised, sore, and fatigued. Arnica is often considered a foundational remedy to address the initial tissue damage and soreness.
Silicea (Silica) may be considered when there is a chronic, lingering case of plantar fasciitis with a tendency toward cold feet, poor circulation, and a feeling that the foot is weak or prone to injury. Individuals who benefit from Silicea are often described as having a delicate constitution and may be prone to slow-healing injuries.
In homeopathic practice, the selection of a remedy is highly individualized. A practitioner will consider not only the physical symptoms—such as the exact location of pain, the modalities (what makes it better or worse), and the sensation—but also the person’s mental and emotional state, sleep patterns, and overall constitution. This holistic approach aligns with the understanding that plantar fasciitis is not an isolated condition but one that interacts with the whole person.
It is crucial to emphasize that homeopathy is not a substitute for conventional medical care. In cases of severe pain, sudden swelling, or if the pain is the result of a traumatic injury, a thorough evaluation by a medical professional is essential. Diagnostic imaging, physical therapy, orthotics, and other conventional treatments play a vital role in managing plantar fasciitis, particularly in moderate to severe cases.
From a homeopathic perspective, these conventional measures are not seen as oppositional but rather as complementary. A person undergoing physical therapy might simultaneously take a homeopathic remedy to support tissue healing and reduce sensitivity to pain. The gentle nature of homeopathic remedies means they can be used alongside other treatments without risk of adverse interactions, though it is always wise to inform all healthcare providers about any therapies being pursued.
Living Well with Plantar Fasciitis
Ultimately, navigating plantar fasciitis requires patience, consistency, and a willingness to listen to one’s body. Recovery is rarely linear; there are often setbacks along the way. However, with a combination of proper support, mechanical care, and a holistic approach to healing, most individuals find significant relief over time.
The journey begins with understanding that the feet are the foundation of the body. When they are compromised, the entire structure is affected. By addressing not only the pain but also the underlying habits, biomechanics, and lifestyle factors that contributed to the condition, one can not only recover but also build resilience against future occurrences.
For those exploring homeopathy, working with a qualified practitioner can open a door to a deeply personalized form of care that honors the individual’s unique experience of illness. Whether used as a primary approach or as part of a broader strategy, homeopathy reminds us that healing involves more than the absence of pain—it involves restoring balance to the whole person.
Frequently Asked Questions About Homeopathic Remedies for Plantar Fasciitis
For those exploring homeopathy as a complementary approach to managing plantar fasciitis, questions naturally arise about how these remedies work, how to use them safely, and what to expect. Below are some of the most common questions, answered in a practical and thoughtful manner.
1. What exactly are homeopathic remedies, and how are they believed to work for plantar fasciitis?
Homeopathic remedies are prepared from natural substances—plants, minerals, or animal products—that undergo a process of serial dilution and vigorous shaking, a process known as potentization. The fundamental principle of homeopathy is “like cures like,” meaning a substance that can produce certain symptoms in a healthy person can, when prepared homeopathically, stimulate the body’s self-healing response to resolve similar symptoms in a person who is unwell.
In the context of plantar fasciitis, a homeopath does not simply prescribe a remedy for “heel pain.” Instead, they match the unique pattern of the individual’s symptoms—such as the nature of the pain (sharp, tearing, bruised), the times it worsens or improves (morning stiffness, relief with movement or with rest), and the person’s overall constitution—to the remedy that most closely mirrors that picture. The goal is to gently nudge the body toward restoring balance and resolving the underlying sensitivity that led to the condition.
2. Are homeopathic remedies safe to use alongside conventional treatments like physical therapy, orthotics, or anti-inflammatory medications?
Yes, homeopathic remedies are generally considered safe to use alongside conventional treatments. Because they are highly diluted, they do not chemically interact with pharmaceutical drugs in the way that herbal supplements or conventional medications might. Many people use homeopathy as a complementary therapy while continuing with physical therapy, stretching routines, orthotic support, or even anti-inflammatory medications.
That said, it is always prudent to inform all your healthcare providers—both conventional and complementary—about any remedies or treatments you are using. If you are taking prescription medications or have underlying health conditions, consulting with a qualified homeopath or your primary care physician before starting a new remedy ensures that your overall care remains coordinated and safe.
3. How do I choose the right homeopathic remedy for my plantar fasciitis?
Choosing the correct remedy is the cornerstone of homeopathic treatment, and it is not as simple as selecting a remedy based solely on the name of the condition. Homeopathy is highly individualized. Two people with plantar fasciitis may receive completely different remedies based on how they experience their pain.
For instance, one person may have pain that is worst when first standing up, improves with continued walking, and feels better from heat—this pattern might point toward Rhus toxicodendron. Another person may have a bruised, sore feeling with tenderness to touch, especially after overexertion, and may benefit from Arnica montana. Someone with chronic, hard swelling and a sensation of ligamentous weakness might be better suited to Calcarea fluorica.
Because of this complexity, working with a trained homeopathic practitioner is highly recommended. They will take a detailed case history, asking about not only your foot pain but also your sleep patterns, energy levels, emotional state, and any other physical complaints, to arrive at a remedy that matches your unique symptom picture.
4. In what potency and dosage should homeopathic remedies be taken for plantar fasciitis?
Homeopathic remedies come in various potencies, such as 6C, 30C, 200C, and higher. The choice of potency and dosage depends on the individual case, the chronicity of the condition, and the sensitivity of the person. For self-care in acute or mild cases, lower potencies like 6C or 30C are often used, taken two to three times daily for a short period. If there is no improvement after a reasonable trial, it is generally advised to stop and seek professional guidance rather than continuing indefinitely.
In more chronic or stubborn cases of plantar fasciitis, a homeopath may prescribe a single dose of a higher potency (such as 200C or 1M) and wait for a period of days or weeks to observe the response. Homeopathy works on the principle of stimulating a healing response, and more is not necessarily better. Overdosing or taking remedies too frequently can sometimes muddy the response. A qualified practitioner can guide you on the appropriate potency and repetition for your specific situation.
5. How long does it take to see results with homeopathic treatment for plantar fasciitis?
The timeline for improvement varies widely. For acute flare-ups—such as plantar fasciitis that developed after a specific incident like a long hike or a sudden increase in running—a well-chosen remedy may bring noticeable relief within hours or days. For chronic, long-standing cases where the condition has been present for months or years, the healing process is typically more gradual. It may take several weeks or even months of consistent treatment to see significant, lasting improvement.
Homeopathy aims to address the underlying susceptibility rather than merely suppressing symptoms. As such, the healing process can sometimes involve a temporary, mild return of old symptoms as the body rebalances—a phenomenon known as a “healing aggravation.” This is generally short-lived and considered a positive sign. Patience and close observation are key, and working with a practitioner helps ensure that the treatment is progressing as intended.
6. Can I use homeopathic remedies preventively if I am prone to plantar fasciitis?
Homeopathy can be used preventively, though the approach is somewhat different. Some individuals who are prone to recurrent plantar fasciitis may benefit from a constitutional remedy—a remedy selected based on their overall physical, emotional, and mental makeup—to strengthen their general resilience. This is often done with the guidance of a homeopath who takes a comprehensive case.
Additionally, certain remedies can be used after activities that tend to trigger symptoms. For example, someone who knows that a long day of standing or an intense workout often leaves their feet sore might take Arnica montana as a supportive measure afterward to reduce inflammation and promote recovery. However, for true prevention, addressing the underlying mechanical causes—such as wearing supportive footwear, stretching regularly, and maintaining a healthy weight—remains essential, with homeopathy serving as a complementary layer of support.
7. Are there any side effects or risks associated with homeopathic remedies for plantar fasciitis?
Homeopathic remedies, when prepared according to recognized pharmacopoeias, are considered extremely safe with a very low risk of adverse effects. Because they are highly diluted, they do not cause toxicity or direct side effects in the manner of conventional drugs. However, it is possible for a remedy to be incorrectly chosen, leading to a temporary worsening of symptoms (a healing aggravation) or simply no effect.
The greater risk lies in self-treating a condition that may require conventional medical attention. If your heel pain is accompanied by fever, redness, significant swelling, numbness, or if it follows a traumatic injury, it is essential to seek evaluation from a medical professional to rule out fractures, infections, or other serious conditions. Homeopathy is best used as a complementary approach, not as a replacement for necessary conventional care.
8. Can I use topical homeopathic creams or gels for plantar fasciitis, and are they effective?
Yes, topical homeopathic preparations are available in the form of creams, gels, and ointments containing ingredients such as Arnica, Ruta, or Calendula. These can be applied directly to the heel and arch area for localized relief. Many people find them soothing, particularly after stretching or at the end of the day.
However, in homeopathic philosophy, topical application is generally considered less powerful than internal administration when the goal is deep, constitutional healing. Topical preparations are often more suited for acute soreness, bruising, or temporary relief. For chronic plantar fasciitis, a homeopath would typically prescribe an internal remedy selected to match the totality of your symptoms, often using the topical product as a supportive adjunct rather than the primary treatment.
9. Should I stop my stretching exercises or physical therapy once I start homeopathic treatment?
No, stretching and physical therapy are vital components of recovering from plantar fasciitis. Homeopathy does not replace the mechanical interventions that address the physical stresses on the plantar fascia. Gentle, consistent stretching of the calf muscles and the plantar fascia itself helps maintain flexibility, reduces tension on the heel, and prevents the condition from recurring.
What homeopathy can do is support the body’s ability to heal from micro-traumas, reduce excessive inflammatory responses, and address any underlying sensitivity or susceptibility that may be prolonging the condition. The two approaches work well in tandem. As you progress, you may find that your tolerance for stretching and activity improves, allowing you to engage more fully in rehabilitation exercises.
10. How do I find a qualified homeopathic practitioner for my plantar fasciitis?
Finding a qualified practitioner is important for safe and effective homeopathic care. Look for professionals who have completed formal training from accredited homeopathic institutions and who hold credentials from recognized professional organizations. In many countries, there are national or regional homeopathic associations that maintain directories of registered practitioners.
When selecting a practitioner, do not hesitate to ask about their experience in treating musculoskeletal conditions like plantar fasciitis. A good homeopath will take a thorough initial case history, which may last an hour or more, and will communicate clearly about their approach, expected timeline, and how they coordinate with other healthcare providers. Many practitioners also offer telemedicine consultations, making it accessible even if there is no local homeopath in your area.
These FAQs aim to provide a balanced, practical overview for those curious about incorporating homeopathy into their journey with plantar fasciitis. As with any healthcare decision, informed choice, professional guidance, and a willingness to listen to your body are the cornerstones of safe and effective care.