Table of Contents
ToggleCellulitis: Causes, Symptoms, Effects, Prevention, and Homeopathic Remedies for Cellulitis
Introduction
Cellulitis is a common but potentially serious bacterial skin infection that affects the deeper layers of the skin, including the dermis and subcutaneous tissue. It is not a condition to be dismissed as a simple rash; without timely and appropriate treatment, it can lead to severe complications. This article provides a detailed exploration of cellulitis, covering its clinical presentation, underlying causes, potential effects on the body, preventive strategies, and an overview of the homeopathic perspective on management. It is crucial to state at the outset that cellulitis is a medical emergency that requires conventional medical intervention, typically antibiotics. The homeopathic information presented here is intended for complementary understanding and should never replace standard medical care.
What is Cellulitis?
Cellulitis occurs when bacteria, most commonly group A Streptococcus or Staphylococcus aureus, enter the skin through a break or crack. Unlike impetigo, which affects the very top layer of skin (the epidermis), cellulitis penetrates deeper, spreading rapidly across the affected area. The infection can occur anywhere on the body, but it most frequently appears on the lower legs, followed by the arms and face. It is characterized by inflammation, pain, and systemic symptoms if the infection becomes severe. The term “cellulitis” should not be confused with “cellulite,” which is a harmless cosmetic condition involving fat deposits beneath the skin.
Symptoms of Cellulitis
The symptoms of cellulitis can range from mild to severe and typically develop quickly, often within 24 hours of the bacteria entering the skin. Recognizing these symptoms early is critical for prompt treatment.
Localized Symptoms on the Skin
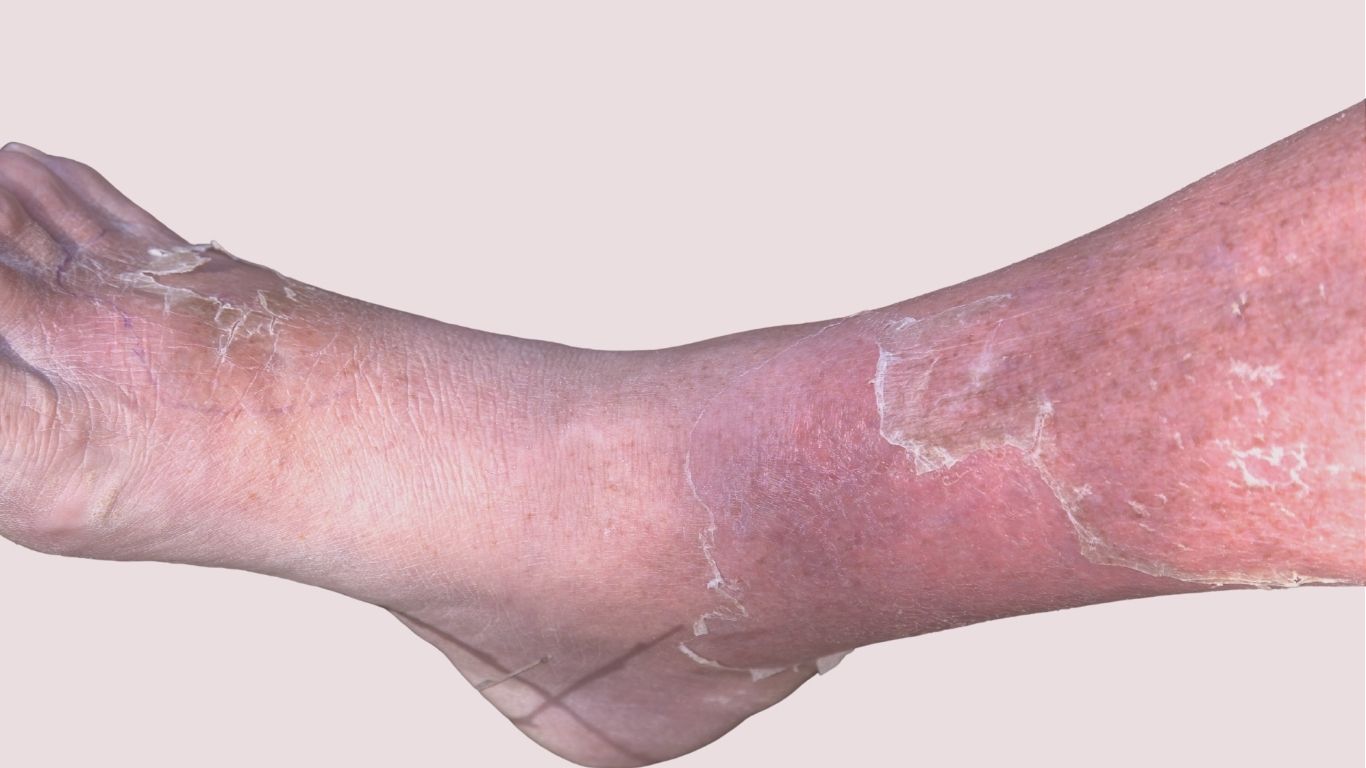
The hallmark of cellulitis is a localized area of skin that becomes red, swollen, and tender. The redness tends to expand as the infection spreads. The affected area often feels warm to the touch, a sign of the body’s inflammatory response. As the infection progresses, the skin may take on a dimpled, orange-peel-like appearance (peau d’orange) due to swelling that affects the hair follicles. In some cases, blisters, bullae (large fluid-filled blisters), or small spots of bleeding under the skin (petechiae) may develop. The affected individual often feels a sensation of tightness or burning in the area.
Systemic Symptoms
As the body fights the infection, systemic symptoms frequently accompany the local signs. These may include:
-
Fever and chills: A high temperature is a common response to a bacterial infection.
-
Malaise: A general feeling of fatigue, weakness, and being unwell.
-
Sweating: Often profuse, especially during fever spikes.
-
Swollen lymph nodes: Lymph nodes near the site of infection, such as in the groin for a leg infection, may become tender and enlarged.
-
Muscle aches and joint stiffness: Particularly in the limb affected.
When to Seek Immediate Medical Attention
Cellulitis can escalate rapidly. Signs that indicate a medical emergency include:
-
A rapid expansion of the red, swollen area.
-
Numbness or loss of sensation in the affected area.
-
High fever with severe chills.
-
Confusion or dizziness, which can be a sign of sepsis (a life-threatening response to infection).
-
The presence of black, dead tissue (gangrene) or large, dark blisters.
Causes and Risk Factors
The primary cause of cellulitis is the entry of bacteria through a breach in the skin barrier. While the skin is a formidable defense, any disruption can serve as an entry point.
Common Bacterial Culprits
The two most common bacteria responsible for cellulitis are:
-
Group A Streptococcus: This is the most frequent cause, especially in non-purulent cellulitis (without abscess formation). It spreads rapidly through the tissues.
-
Staphylococcus aureus: This bacterium is another common cause, particularly in cases associated with wounds, abscesses, or surgical sites. Methicillin-resistant Staphylococcus aureus (MRSA) is a growing concern and can lead to more difficult-to-treat infections.
Other bacteria, such as Haemophilus influenzae (more common in children, causing facial cellulitis), Pasteurella multocida (from animal bites), and gram-negative bacteria, can also be causative agents in specific circumstances.
Portals of Entry
The bacteria require a break in the skin to invade. Common portals of entry include:
-
Cuts, scrapes, and surgical wounds: Even minor injuries like a paper cut can be sufficient.
-
Insect bites and stings: Mosquito, spider, or other insect bites can introduce bacteria when scratched.
-
Athlete’s foot (tinea pedis): This is a significant risk factor, especially for cellulitis of the lower leg. The fungal infection causes cracks and fissures between the toes, creating a direct pathway for bacteria.
-
Chronic skin conditions: Eczema, psoriasis, and dermatitis compromise the skin’s integrity.
-
Ulcers: Venous stasis ulcers or diabetic foot ulcers are chronic wounds prone to infection.
-
Intravenous drug use: Needle puncture sites are high-risk portals.
Risk Factors
Certain individuals are at a higher risk of developing cellulitis. These include:
-
Lymphedema: Chronic swelling of an arm or leg due to damaged or removed lymph nodes (common after cancer surgery) significantly increases risk, as the lymphatic system is crucial for fighting infection.
-
Chronic venous insufficiency: Poor circulation in the veins of the legs leads to swelling, skin changes, and a predisposition to breaks in the skin.
-
Obesity: Excess weight can impair circulation and lymphatic drainage, and increase the risk of skin folds that can harbor moisture and bacteria.
-
Diabetes mellitus: High blood sugar can impair immune function, delay wound healing, and increase the risk of neuropathy, where a person may not feel a minor injury that then becomes infected.
-
Weakened immune system: Individuals undergoing chemotherapy, taking immunosuppressive medications, or living with HIV/AIDS are more susceptible.
-
Previous history of cellulitis: Having had cellulitis before dramatically increases the risk of recurrence, often in the same location.
Effects and Potential Complications
When treated promptly with appropriate antibiotics, the effects of cellulitis are usually limited to the acute illness. However, if left untreated or if treatment fails, the infection can lead to severe and lasting consequences.
Local and Regional Spread
The infection can spread from the skin to deeper structures. Necrotizing fasciitis, also known as “flesh-eating disease,” is a rare but devastating complication where the infection destroys soft tissue, including fascia (the connective tissue that surrounds muscles). This is a surgical emergency. Another complication is suppurative arthritis (septic arthritis) or osteomyelitis (bone infection), where the bacteria spread from the skin to adjacent joints or bones.
Systemic Complications
The most dangerous effect of untreated cellulitis is sepsis. This occurs when the body’s response to the infection causes widespread inflammation, leading to blood clots, leaky blood vessels, and organ failure. Sepsis is a life-threatening condition that requires intensive care.
Chronic Effects and Sequelae
Even after successful treatment, cellulitis can have lasting effects:
-
Recurrent cellulitis: Damage to the lymphatic vessels during an initial infection can lead to chronic lymphedema, which in turn creates a cycle of recurrent infections. Each subsequent episode can cause further lymphatic damage.
-
Chronic swelling: Permanent swelling of the affected limb is a common long-term effect.
-
Post-cellulitis changes: The skin may remain discolored, thickened, or prone to dryness and cracking, perpetuating the risk of recurrence.
Prevention Strategies
Given the high rate of recurrence, prevention is a cornerstone of cellulitis management, especially for those with known risk factors.
Skin Care and Hygiene
The first line of defense is meticulous skin care. This includes:
-
Moisturizing regularly: Keeping skin hydrated prevents cracks and fissures, particularly on dry heels and between the toes. Using a fragrance-free, high-quality moisturizer daily is essential.
-
Prompt wound care: Any cut, scrape, or insect bite should be cleaned immediately with soap and water. Applying a topical antibiotic ointment and covering with a sterile bandage until healed can prevent bacterial entry.
-
Managing fungal infections: Prompt treatment of athlete’s foot with antifungal creams or powders is crucial. Keeping feet clean and dry, and wearing breathable footwear, can help prevent this common portal of entry.
-
Nail care: Keeping fingernails and toenails trimmed and clean reduces the risk of introducing bacteria through scratching or from hangnails.
Management of Underlying Conditions
Controlling predisposing conditions is vital:
-
Lymphedema management: For individuals with lymphedema, wearing prescribed compression garments, performing manual lymphatic drainage, and exercising can reduce swelling and the risk of infection.
-
Diabetes control: Maintaining optimal blood glucose levels supports immune function and wound healing.
-
Weight management: Achieving and maintaining a healthy weight reduces strain on the circulatory and lymphatic systems.
Lifestyle and Precautions
-
Avoiding skin trauma: For those with a history of cellulitis in a limb, avoiding activities that could lead to injury in that limb is prudent.
-
Proper footwear: Wearing protective, well-fitting shoes to prevent minor foot injuries is important, especially for individuals with diabetic neuropathy.
Homeopathic Treatment: A Complementary Perspective
Homeopathy is a system of alternative medicine based on the principle of “like cures like”—the idea that a substance that causes symptoms in a healthy person can, in a highly diluted form, treat similar symptoms in a sick person. It is important to approach this topic with clarity: there is no robust scientific evidence from randomized controlled trials to support the use of homeopathy as a primary treatment for bacterial infections like cellulitis. Relying solely on homeopathy for a condition that can lead to sepsis is dangerous. However, some individuals seek homeopathic remedies as a complementary approach to support the body’s healing process alongside conventional antibiotics, or for managing predisposing conditions and preventing recurrence. The following information is based on homeopathic materia medica and traditional practice. It is not a substitute for antibiotics or emergency medical care.
In homeopathy, treatment is highly individualized. A homeopath would not simply prescribe a remedy for “cellulitis” but would select a remedy based on the totality of the person’s symptoms—the location, the nature of the pain, the appearance of the affected skin, the person’s mental state, and their unique constitution.
Commonly Indicated Homeopathic Remedies
Several remedies are frequently considered in cases of cellulitis and skin infections. Their descriptions are based on classical homeopathic literature.
Apis mellifica (Apis)
This remedy is derived from the honeybee. It is often indicated for cellulitis that presents with intense swelling, stinging or burning pain, and a sensation of heat. The affected area is typically rosy or pink, and the swelling is such that the skin looks shiny and feels tight. The individual may feel worse from heat and touch and may find relief from cold applications. This is often considered for early-stage infections with a sudden onset, especially those resembling a severe allergic reaction or insect bite reaction that has become infected.
Belladonna
Belladonna is indicated for conditions with a sudden, violent onset. The infection is characterized by intense, throbbing pain, a fiery red color, and heat radiating from the area. The skin is hot, dry, and often looks bright red. The individual may have a high fever, a flushed face, and dilated pupils. It is typically considered for the very early, inflammatory stage before any pus formation. Symptoms are often worse from touch, jarring, or lying on the affected side.
Hepar sulphuris calcareum (Hepar sulph.)
This remedy is often considered when the infection is progressing towards suppuration (abscess formation). It is indicated for extreme sensitivity to pain and touch—the area is exquisitely tender. The individual may be very irritable and chilly. The skin condition is often described as having a splinter-like sensation. Hepar sulph is thought to help “bring to a head” and resolve abscesses or prevent the spread of infection to surrounding tissues.
Silicea (Silica)
Silica is a deep-acting remedy often indicated for chronic, lingering infections or for individuals with a tendency to recurrent cellulitis or abscesses. It is considered when there is poor wound healing, or when the body struggles to expel foreign matter or infectious material. The individual may be chilly, timid, and prone to low stamina. Silica is frequently prescribed constitutionally to strengthen the body’s response to infection and prevent recurrences.
Lachesis mutus (Lachesis)
This remedy is derived from the bushmaster snake venom. It is indicated for infections that are purplish, bluish, or dark red in color, with a tendency to spread rapidly. The infection often starts on the left side or moves from left to right. The individual may feel worse from tight clothing, pressure, and during sleep. It is sometimes considered for severe cases with a septic or hemorrhagic tendency.
Arnica montana (Arnica)
Arnica is well-known for its use in trauma. It is not a remedy for the infection itself but may be used adjunctively to address the sore, bruised, and tender feeling that often accompanies cellulitis. It is thought to help reduce the risk of secondary infection after an injury and is sometimes used to manage the “shock” to the tissues.
The Role of the Homeopath
A qualified homeopath takes a detailed case history, considering not only the physical symptoms but also the person’s emotional state, sleep patterns, food cravings or aversions, and overall constitution. The goal is to find a single remedy that matches the entire symptom picture, stimulating the body’s own healing response. For an acute condition like cellulitis, a homeopath would work alongside a medical doctor, never in place of one.
A Critical Note on Safety and Integration
It cannot be overstated that cellulitis is a bacterial infection that can spread to the bloodstream with life-threatening consequences. Antibiotics are the proven, life-saving standard of care. Homeopathic remedies do not contain measurable amounts of active antibacterial agents and should never be used to delay or replace antibiotic therapy. The appropriate integration is to use homeopathy as a supportive measure—for instance, to manage the inflammatory response alongside antibiotics, or to address constitutional weaknesses that predispose a person to recurrent infections, always under the supervision of a qualified practitioner who understands the gravity of the condition.
Frequently Asked Questions About Homeopathic Remedies for Cellulitis
1. Can homeopathy cure cellulitis on its own?
No. Cellulitis is a bacterial infection that spreads rapidly through the deep layers of the skin. Without prompt treatment with antibiotics, it can lead to serious complications such as abscess formation, sepsis, or even life-threatening systemic infection. Homeopathic remedies are highly diluted substances that do not contain measurable antibacterial agents. While they are sometimes used as a complementary support, they should never replace conventional medical treatment. If you suspect cellulitis, seeking immediate care from a medical professional for antibiotics is essential.
2. How can homeopathy be used alongside antibiotics?
For individuals who choose to explore homeopathy, it is typically used as a supportive measure rather than a primary treatment. Some people find that certain homeopathic remedies help manage the inflammatory response—such as reducing swelling, throbbing pain, or the sensation of heat—while antibiotics work to eradicate the bacterial infection. Others use homeopathy to address underlying constitutional weaknesses, such as poor lymphatic drainage or recurrent skin infections, in an effort to reduce the likelihood of future episodes. Any use of homeopathy should be discussed with both a qualified homeopath and the prescribing medical doctor to ensure safe and coordinated care.
3. Are homeopathic remedies safe to take with antibiotics?
Homeopathic remedies are generally considered safe when used alongside conventional medications because they are prepared in highly diluted forms that do not chemically interact with pharmaceutical drugs. However, safety depends on responsible use. The greater risk lies not in the interaction of the substances but in the potential for a person to delay or forgo antibiotics in favor of homeopathy alone. If you are taking antibiotics for cellulitis, adding a homeopathic remedy under the guidance of a trained practitioner is unlikely to cause harm, but it should never be done with the intention of replacing the antibiotic course.
4. How do I choose the right homeopathic remedy for cellulitis?
In homeopathy, remedy selection is highly individualized. A practitioner does not simply match a remedy to a disease name—such as cellulitis—but instead matches a remedy to the unique symptom picture of the person. This includes the specific characteristics of the infection: the color of the skin (bright red, purplish, or dusky), the type of pain (throbbing, stinging, burning, or splinter-like), the presence and nature of swelling, whether the person feels better or worse from heat or cold, and even the person’s emotional state. For this reason, self-prescribing is often discouraged. A qualified homeopath takes a detailed case history to select a single remedy that fits the totality of symptoms.
5. What are the most commonly indicated homeopathic remedies for skin infections like cellulitis?
Several remedies appear frequently in homeopathic literature for skin infections. Apis mellifica is often considered for intense swelling with stinging pain and heat, where the skin appears rosy and feels better from cold. Belladonna is associated with sudden onset, fiery redness, throbbing pain, and high fever. Hepar sulphuris is indicated when the area is exquisitely tender and the infection is threatening to form an abscess. Silicea is often used constitutionally for individuals with poor wound healing or a tendency toward recurrent infections. Lachesis may be considered for infections with a purplish or dark appearance that spread rapidly. Again, these are general indications, and proper selection requires professional assessment.
6. Can homeopathy help prevent recurrent cellulitis?
One of the more common reasons people seek homeopathic care in the context of cellulitis is to address recurrent episodes. After a first episode, damage to the lymphatic vessels can lead to chronic swelling (lymphedema), which significantly increases the risk of future infections. Homeopaths often focus on constitutional treatment—prescribing a remedy based on the person’s overall physical, emotional, and medical history—with the goal of strengthening the body’s immune response, improving tissue resilience, and supporting lymphatic function. While some individuals report fewer recurrences with this approach, it is important to continue all conventional preventive measures, such as compression therapy, skin hydration, and management of underlying conditions like diabetes or venous insufficiency.
7. How quickly do homeopathic remedies work for an acute infection?
In homeopathic theory, if a well-selected remedy matches the acute symptom picture, improvements may be noticed within hours in terms of reduced pain, swelling, or fever. However, this is highly variable. For a condition as serious as cellulitis, any perceived improvement should not be interpreted as a sign that antibiotics are unnecessary. The infection can continue to spread internally even if surface symptoms appear to be improving. A responsible approach is to monitor symptoms closely under medical supervision and to complete the full course of prescribed antibiotics regardless of any concurrent homeopathic treatment.
8. Are there any risks associated with using homeopathy for cellulitis?
The primary risk is not from the remedies themselves, which are generally regarded as safe, but from the potential for misuse or misunderstanding. Delaying or refusing conventional antibiotic treatment for cellulitis in favor of homeopathy can have life-threatening consequences, including the rapid progression of infection to sepsis, necrotizing fasciitis, or osteomyelitis. Additionally, applying topical homeopathic creams or lotions to an open or infected wound without proper medical evaluation can introduce further irritation or obscure the clinical picture for the treating physician. Homeopathy should be viewed as a complementary support, not a standalone treatment for bacterial infections.
9. Should I see a homeopath during an active cellulitis infection?
If you wish to incorporate homeopathy into your care, it is safest to do so in consultation with both a medical doctor and a qualified homeopath. During an acute infection, a homeopath can assess your symptoms and suggest a remedy that may help manage discomfort alongside your antibiotic treatment. However, the priority must always be the timely initiation of antibiotics. Once the acute infection is resolved, a homeopath may focus on constitutional treatment to address underlying vulnerabilities and support long-term prevention. Always inform both your doctor and your homeopath about all treatments and remedies you are using.
10. Is there scientific evidence supporting homeopathy for cellulitis?
Current scientific literature does not provide robust evidence from large-scale randomized controlled trials to support the use of homeopathy as an effective treatment for bacterial infections such as cellulitis. The consensus within mainstream medicine is that antibiotics are the only evidence-based treatment for this condition. Homeopathy operates on principles that differ fundamentally from conventional pharmacology, and its effects are not explained by the same mechanisms as pharmaceutical drugs. Individuals who choose to explore homeopathy typically do so based on personal experience, tradition, or a preference for a holistic approach, but this choice should be made with full awareness of the proven necessity of conventional medical treatment for cellulitis.
Conclusion
Cellulitis is a serious bacterial infection of the deep skin layers that demands respect and prompt medical attention. Its symptoms—rapidly spreading redness, swelling, heat, and pain—can escalate quickly, leading to complications like abscess formation, lymphedema, and life-threatening sepsis. Understanding the causes, from minor skin breaks to chronic conditions like lymphedema and diabetes, is key to prevention. Meticulous skin care, management of underlying health issues, and prompt wound care form the foundation of prevention. While conventional antibiotics remain the cornerstone of treatment, a supportive approach that includes proper wound care, elevation, and rest is essential. For those interested in holistic health, homeopathy offers a complementary framework aimed at supporting the body’s resilience and addressing individual susceptibilities. However, it must be used with caution and only in conjunction with, never in place of, evidence-based medical treatment. Recognizing the signs of cellulitis early and seeking immediate conventional care is the single most important step anyone can take to ensure a full and uncomplicated recovery.