Table of Contents
ToggleDeep Vein Thrombosis (DVT): Understanding Symptoms, Causes, Effects, Prevention, and Effective Homeopathic Remedies for Deep Vein Thrombosis.
Introduction
Deep vein thrombosis, often shortened to DVT, is a medical condition that doesn’t always announce itself with fanfare. In fact, it is frequently called a “silent killer” because its first sign can be a sudden, life-threatening event. At its core, DVT is the formation of a blood clot, known as a thrombus, within one of the deep veins of the body. While these clots can develop anywhere, they most commonly occur in the lower leg, thigh, or pelvis. Understanding this condition is not just about knowing a medical term; it is about recognizing a potential danger that can affect anyone, from a person recovering from surgery to an office worker sitting at a desk for hours.
The real danger of DVT lies not always in the clot itself, but in what it can do if it breaks free. When a piece of the clot dislodges, it travels through the venous system, heading toward the heart and then into the pulmonary arteries in the lungs. This complication is called a pulmonary embolism (PE), and it can block blood flow to the lungs, causing severe damage or even death. This is why DVT is considered a medical emergency, and awareness of its signs is a crucial life skill.
Recognizing the Symptoms and Understanding the Causes
The symptoms of DVT can be deceptive because they mimic other, less serious conditions. Some people experience no symptoms at all, while others have unmistakable signs. The classic presentation usually involves one leg, rarely both. The most common symptoms include swelling in the affected leg, which may be sudden and significant. Alongside swelling, there is often pain or tenderness that feels like a cramp or a persistent soreness, typically starting in the calf. The skin over the affected area might feel warmer to the touch than the surrounding skin, and it can change color, appearing pale, reddish, or even taking on a bluish tint. It is vital to note that a DVT is not the same as a superficial blood clot you can see just under the skin, like those in varicose veins. The deep veins are hidden, so the symptoms are internal.
However, a large number of DVTs are asymptomatic, which is what makes them so treacherous. The first clue might be a pulmonary embolism, which has its own alarming signs: sudden shortness of breath, sharp chest pain that worsens with deep breathing, a rapid heart rate, coughing up blood, or feeling faint and lightheaded. If any of these occur, immediate medical attention is non-negotiable.
So, why do these clots form in the first place? The underlying causes are often described by what doctors call Virchow’s Triad, three key factors that contribute to abnormal clotting. The first is stasis of blood flow, meaning the blood is moving too slowly or pooling in the veins. This happens during long periods of immobility, such as long-haul flights, bed rest after surgery, or even sitting at a desk for a full workday without moving your legs. The second factor is endothelial injury, which is damage to the inner lining of the blood vessel. This can result from trauma, fractures, surgery (especially orthopedic procedures on the hips or knees), or even from indwelling catheters placed in the veins. The third factor is hypercoagulability, a state where the blood has a higher tendency to clot. This can be an inherited condition, such as Factor V Leiden mutation, or an acquired one, such as from cancer, pregnancy, the use of oral contraceptives or hormone replacement therapy, or chronic inflammatory diseases.
Beyond the triad, several other risk factors increase a person’s likelihood of developing DVT. Age is a major one, as the risk rises significantly after 40. Obesity adds mechanical pressure on the veins in the pelvis and legs, slowing circulation. A personal or family history of DVT or PE is another strong indicator. Conditions like heart failure and inflammatory bowel disease also elevate the risk. Understanding these causes is the first step in shifting from a reactive to a proactive approach to health.
The Immediate and Long-Term Effects on the Body
The effects of DVT can be divided into two categories: immediate, potentially fatal complications and long-term, chronic disabilities. The most immediate and feared effect is pulmonary embolism. When a clot travels to the lungs, it blocks the pulmonary arteries, which are responsible for carrying deoxygenated blood to the lungs to pick up fresh oxygen. A large clot can cause a massive PE, leading to a sudden drop in blood pressure, shock, and cardiac arrest. Even a smaller PE can cause damage to lung tissue, leading to a pulmonary infarction, where a portion of the lung dies due to lack of blood. Surviving a PE is a harrowing experience and often requires prolonged treatment with blood thinners and close monitoring of heart and lung function.
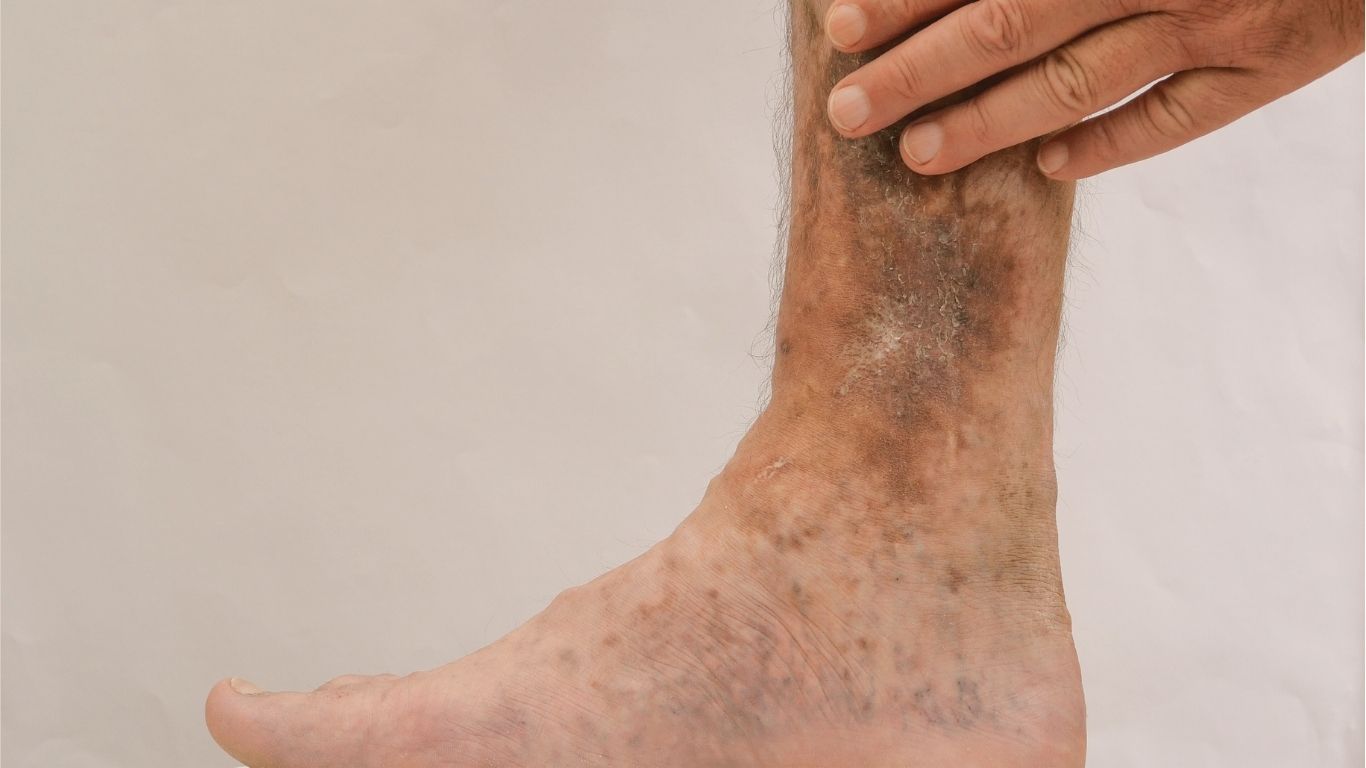
But even if a DVT never progresses to a PE, it can still cause significant long-term damage. A frequent consequence is a condition called post-thrombotic syndrome (PTS). This develops because the clot damages the delicate one-way valves inside the deep veins. Normally, these valves prevent blood from flowing backward down the leg. When they are destroyed by inflammation and scarring from the clot, blood pools in the lower leg, a condition known as venous insufficiency. The symptoms of PTS can be debilitating. They include chronic leg swelling, a heavy or aching sensation that worsens as the day goes on, skin changes such as hardening or darkening (stasis dermatitis), and in severe cases, painful venous ulcers that are difficult to heal. These ulcers often develop around the ankle and can persist for months, severely impacting a person’s mobility and quality of life. Treating PTS is challenging and focuses on compression therapy, leg elevation, and wound care, but the damage to the valves is largely irreversible. Therefore, preventing the initial DVT is far better than dealing with its aftermath.
Practical Strategies for Prevention
Preventing DVT is a blend of lifestyle awareness and specific medical strategies, especially for those at high risk. For the average person, the most powerful prevention tool is movement. The calf muscles act as a secondary heart for the legs; when they contract during walking or flexing, they squeeze the deep veins and push blood upward toward the chest. Simple actions can make a huge difference. On long car or plane journeys, make a point to stop and walk every hour. While seated, perform ankle pumps—pointing your toes up and down—and circle your feet. Stay well-hydrated with water, as dehydration can make blood slightly thicker and more prone to clotting. Avoid alcohol and sedatives during long trips, as they lead to immobility and poor posture.
For those who are bedridden after surgery or illness, preventive measures are even more critical. Hospitals routinely use intermittent pneumatic compression devices—sleeves that wrap around the legs and automatically inflate and deflate to mimic the pumping action of muscles. Graduated compression stockings are also commonly prescribed. These are not ordinary socks; they are tightest at the ankle and gradually loosen up the leg, which helps push blood upward and prevents pooling. For patients at very high risk, such as those undergoing hip or knee replacement, doctors will often prescribe prophylactic anticoagulant medications, like low-molecular-weight heparin injections, to temporarily keep the blood from clotting too easily.
Lifestyle modifications also play a large role in long-term prevention. Maintaining a healthy weight reduces pressure on the pelvic and leg veins. Regular exercise, especially walking, swimming, or cycling, promotes excellent venous circulation. For women, discussing the risks of oral contraceptives or hormone therapy with a doctor is important, especially if they have other risk factors like a family history of clots or smoking. Smoking cessation is crucial, as smoking damages blood vessel walls and increases clotting factors. Lastly, if you have a known inherited clotting disorder, working closely with a hematologist to create a personalized prevention plan is essential, particularly during high-risk periods like pregnancy or surgery.
The Homeopathic Perspective: A Complementary Approach
It is important to state clearly from the outset that homeopathy is a system of alternative medicine based on the principle of “like cures like,” using highly diluted substances. There is no robust scientific evidence from large-scale, peer-reviewed clinical trials to support the use of homeopathic remedies as a standalone treatment for an acute DVT. Using homeopathy to treat a confirmed DVT instead of standard medical therapies like anticoagulants (blood thinners) is dangerous and can lead to clot progression, pulmonary embolism, or death. Standard medical treatments are proven, life-saving, and should never be delayed or replaced by homeopathy.
However, some individuals and practitioners of homeopathy discuss its potential role in a complementary manner—that is, as an adjunct to conventional care, or for managing the residual symptoms and long-term effects like post-thrombotic syndrome. From this perspective, homeopathic remedies are chosen based on the individual’s specific symptom picture, not just the disease name. A homeopath would ask detailed questions about the nature of the pain, the appearance of the swelling, the person’s constitution, and any factors that make symptoms better or worse. The following are some remedies that homeopathic literature cites for conditions resembling venous congestion or the aftermath of clotting. Again, these are not treatments for an active DVT.
Arnica montana is often the first remedy considered for any trauma or injury to the veins. It is associated with a feeling of being bruised and sore, as if the person has been beaten. In the context of DVT risk, a homeopath might consider it after surgery or an injury to the leg where there is a fear of clot formation, but always alongside standard prophylactic measures.
Hamamelis virginiana, derived from the witch-hazel plant, is known in homeopathy for its affinity for the venous system. It is indicated for varicose veins and for a heavy, bruised feeling in the legs. The person needing Hamamelis may have bleeding tendencies or a feeling of fullness and congestion in the veins. It is sometimes mentioned for the early stages of venous inflammation.
Lachesis mutus, made from the venom of the bushmaster snake, is a deep-acting remedy often linked to circulatory issues. The key indications for Lachesis include a left-sided tendency, symptoms that are worse from pressure or tight clothing around the neck or waist, and a purplish or bluish discoloration of the skin. In homeopathic theory, it might be considered for a DVT that is very painful and involves a dark, swollen extremity.
Vipera torva, or common viper venom, is another remedy specifically associated with venous stasis. The person who needs Vipera typically has a leg that is hugely swollen, blue, and intensely painful. The hallmark feature is that the pain is unbearable when the leg is hanging down but is almost instantly relieved when the leg is elevated. This “dependency” modality is very specific. Vipera is sometimes discussed in the context of acute phlebitis or deep vein inflammation.
Finally, Fluoric acid is often indicated for the long-term consequences of venous damage, including chronic leg ulcers and the hard, indurated (hardened) veins seen in post-thrombotic syndrome. The person needing Fluoric acid may feel better with cold applications and worse with heat, and they often have a tendency to tissue breakdown and poor healing.
The role of homeopathy in DVT is not as a cure or a substitute for emergency medicine. If you suspect a DVT—with leg swelling, pain, and warmth—the only correct course of action is to go to an emergency room or urgent care center immediately for a Doppler ultrasound and, if necessary, anticoagulation therapy. After the acute danger has passed and you are under the care of a medical doctor, some individuals explore homeopathy to help manage chronic discomfort, swelling, or the emotional after-effects of a serious health scare. This should always be done transparently and collaboratively with both your medical doctor and a qualified, registered homeopath.
FAQs About Homeopathic Remedies for Deep Vein Thrombosis
1. Can homeopathic remedies alone cure an acute deep vein thrombosis?
No. This is the most important question to address. There is no scientific evidence or clinical consensus that homeopathic remedies, taken alone, can dissolve an existing blood clot or prevent a pulmonary embolism. An acute DVT is a medical emergency that requires immediate diagnosis (usually via ultrasound) and rapid treatment with conventional anticoagulants (blood thinners) such as heparin, warfarin, or direct oral anticoagulants. Relying solely on homeopathy for an active DVT can lead to clot extension, permanent vein damage, or fatal pulmonary embolism. Homeopathy should never replace standard emergency or long-term medical care for DVT.
2. If homeopathy can’t cure DVT, why do some people use it?
Some individuals use homeopathic remedies in a complementary role, alongside conventional medical treatment. After the acute clot has been stabilized with anticoagulants, and under a doctor’s supervision, a homeopath may suggest remedies to address lingering symptoms or the after‑effects of DVT. These include chronic leg swelling, heaviness, skin discoloration, or pain from post‑thrombotic syndrome. Others turn to homeopathy for emotional support after a traumatic health event like a pulmonary embolism. However, the primary, non‑negotiable treatment for DVT itself remains conventional medicine.
3. Which homeopathic remedies are most often mentioned for venous issues, and what are they supposed to do?
Homeopathic literature cites several remedies for conditions resembling venous congestion or the aftermath of clotting. None of these should be used to treat an active clot, but they are sometimes discussed for symptom management in chronic cases.
-
Arnica montana: Often associated with trauma or injury to blood vessels. In theory, it might be considered after surgery or a leg injury when there is concern about vein damage, but it does not dissolve clots.
-
Hamamelis virginiana: Linked to a heavy, bruised feeling in the legs and used for varicose veins or superficial phlebitis. It is not a treatment for deep vein thrombosis.
-
Lachesis mutus: Typically indicated for circulatory issues with a purplish discoloration, left‑sided symptoms, and sensitivity to pressure. Some homeopaths consider it for swollen, painful extremities, but again, not as a clot‑buster.
-
Vipera torva: Known for intense leg swelling and pain that is worse when the leg hangs down and better when elevated. This symptom picture matches severe venous stasis, but the remedy does not replace compression or anticoagulation.
-
Fluoric acid: Sometimes mentioned for chronic, non‑healing venous ulcers and hardened veins seen in long‑standing post‑thrombotic syndrome.
These remedies are chosen based on an individual’s complete symptom picture, not on the disease name alone. They are highly diluted and work on energetic principles not recognized by conventional pharmacology.
4. Is it safe to take homeopathic remedies while on prescription blood thinners?
Generally, homeopathic remedies prepared according to standard pharmacopoeias are extremely dilute and contain negligible amounts of the original substance. They are unlikely to interact pharmacologically with anticoagulants like warfarin, apixaban, or rivaroxaban. However, two important cautions exist. First, some homeopathic preparations sold as “mother tinctures” or low dilutions (e.g., 1X, 2X) may contain trace amounts of plant or mineral substances that could theoretically affect bleeding time. Second, any change in your perceived well‑being should never lead you to alter or stop your prescribed blood thinners. Always inform your medical doctor and your homeopath about all remedies and medications you are taking. Never self‑prescribe homeopathic remedies for a condition as serious as DVT.
5. Can homeopathy help prevent DVT in high‑risk situations, like long flights or after surgery?
There is no reliable evidence that homeopathic remedies prevent clot formation in high‑risk scenarios. For long flights, proven prevention includes moving every hour, doing ankle pumps, staying hydrated, and avoiding alcohol. For post‑surgical prevention, hospitals use compression devices, stockings, and prophylactic anticoagulant shots. Relying on a homeopathic remedy in these situations would be unwise. If you are interested in homeopathy for general circulatory support, it should be an addition to, not a replacement for, these evidence‑based measures. Speak with your doctor first.
6. How do I choose the right homeopathic remedy for post‑thrombotic syndrome?
You should not choose a remedy on your own based solely on a list of names. Homeopathy is highly individualized. A qualified, registered homeopath will take a detailed case history, asking about the exact sensation of the leg pain (burning, bursting, stitching), what makes it better or worse (heat, cold, elevation, movement), your overall energy levels, sleep patterns, and emotional state. For example, one person with chronic leg swelling might receive Vipera because the pain is worse when the leg hangs down, while another might receive Fluoric acid because they have hard, ulcerated skin. An online search or a friend’s recommendation is not a substitute for a professional consultation.
7. Are there any risks to using homeopathy for DVT‑related symptoms?
The primary risk is not from the remedies themselves, which are generally very safe due to high dilution, but from the potential for delay or replacement of effective care. The biggest danger is a person deciding to treat a new or recurrent leg swelling with a homeopathic remedy instead of going to the emergency room. That delay can be fatal. A secondary risk is that someone might stop their prescribed anticoagulants because they feel better after taking a homeopathic remedy, leading to a recurrent clot. Always use homeopathy as a complementary tool, not as a substitute for conventional medical monitoring and treatment.
8. What should I do if I have a history of DVT and want to explore homeopathy?
First, ensure your DVT is fully managed by a medical doctor. You should have regular follow‑ups, including blood tests if you are on warfarin, and clear instructions on what to do if symptoms return. Second, find a registered homeopath who is willing to communicate with your doctor. Be transparent about your medical history, all medications, and any current symptoms. Third, treat homeopathy as an experiment in managing residual discomfort or quality of life, not as a cure for the underlying clotting tendency. If you experience any new swelling, warmth, or pain in your leg, go to the emergency room immediately, regardless of what homeopathic remedy you have taken. Your life depends on it.
Conclusion
Deep vein thrombosis is a condition that demands respect. It is a bridge between a seemingly benign leg cramp and a fatal pulmonary embolism. Its causes—stagnation, injury, and hypercoagulability—are present in many modern lifestyles, from the office worker to the long-haul traveler. The effects can be immediate and catastrophic or slow and debilitating, leading to a lifetime of leg pain and ulcers. The good news is that prevention is highly effective. Simple acts like walking, ankle pumps, hydration, and weight management can save lives. For those at higher risk, medical prophylaxis with compression devices or medications is a proven strategy. When it comes to treatment, standard medical care with anticoagulants is non-negotiable for saving life and limb. While homeopathic remedies may be of theoretical interest for constitutional support or managing chronic post-thrombotic symptoms, they have no place in the acute treatment of a blood clot. The most important takeaway is awareness: listen to your legs, move your body, and never ignore sudden, unexplained swelling or pain. In the case of DVT, a moment of vigilance can mean the difference between a simple recovery and a tragedy.
2 thoughts on “Homeopathic Remedies for Deep Vein Thrombosis”