Table of Contents
ToggleFistula: Symptoms, Causes, Effects, Prevention and Homeopathic Remedies for Fistula
Introduction
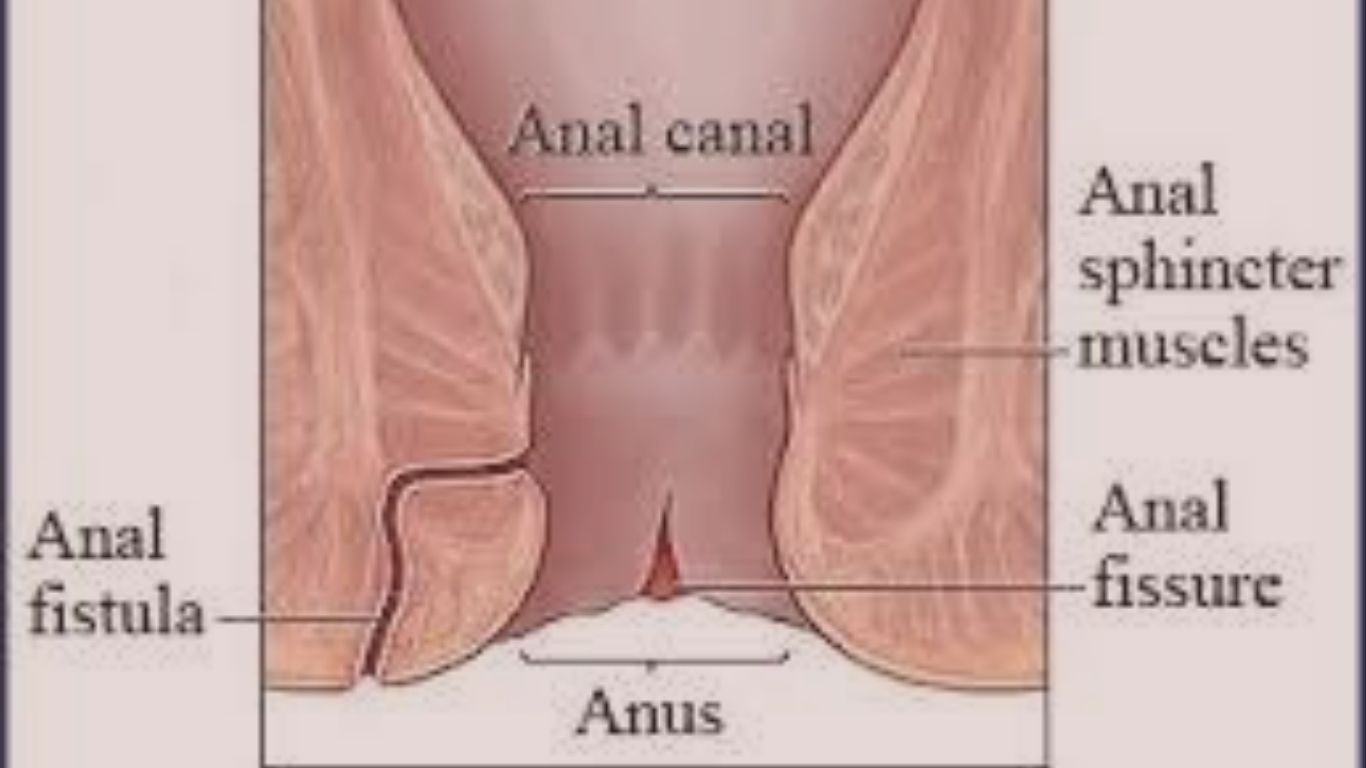
A fistula is one of those medical conditions that people often hesitate to talk about, largely due to its location and the embarrassing nature of its symptoms. Yet, it is far more common than many realize, affecting thousands of individuals worldwide and causing significant physical discomfort and emotional distress. In simple terms, a fistula is an abnormal, tunnel-like connection that forms between two organs or between an organ and the skin surface. These passages are not supposed to exist in a healthy body. They can develop in various parts of the body, but the most frequently encountered type in clinical practice is the anal fistula, which connects the anal canal or rectum to the skin near the anus. Other types include vaginal fistulas, urinary tract fistulas, and enterocutaneous fistulas.
The formation of a fistula is almost always a sign that something has gone wrong inside the body, usually following an infection, inflammation, or injury. To understand the condition fully, one must look at why fistulas form, what warning signs they present, how they affect daily life, what steps can be taken to avoid them, and what treatment options exist, including the role of homeopathic medicine.
Recognizing the Symptoms of a Fistula
The symptoms of a fistula depend largely on its location, but there are several common threads that run through most cases. For anal fistulas, which are the focus of this discussion due to their prevalence, the symptoms are often unmistakable once they appear. The most typical sign is persistent drainage from an opening near the anus. This discharge may consist of pus, blood, or a foul-smelling fluid, and it often stains undergarments, leading to considerable embarrassment. The drainage tends to be worse after a bowel movement.
Pain is another hallmark symptom. Unlike a sharp, stabbing pain, fistula-related pain is often described as a dull, throbbing ache that worsens when sitting down, moving around, or during defecation. Interestingly, when the fistula drains freely, the pain may temporarily subside. However, if the external opening of the fistula heals over before the internal infection has cleared, the pus and bacteria become trapped. This leads to the formation of a painful abscess, causing swelling, redness, and intense tenderness in the area. Other systemic signs such as fever, chills, and a general feeling of being unwell can also appear during these acute flare-ups. Irritation of the skin surrounding the anus, including itching and a rash, is also common due to the constant moisture and chemical irritation from the discharge.
In the case of other fistulas, the symptoms vary widely. A vesicovaginal fistula, for instance, which connects the bladder to the vagina, typically causes continuous, involuntary leakage of urine. A rectovaginal fistula, connecting the rectum and vagina, results in the passage of gas or stool through the vagina. These symptoms are profoundly distressing and can lead to social isolation if not addressed.
Digging into the Causes of Fistula
Understanding why a fistula forms requires a look at the underlying processes of infection and inflammation. In the vast majority of cases, an anal fistula begins with an anal abscess. Anal glands located inside the anal canal can become blocked, leading to a bacterial infection. The body’s natural response is to form an abscess, a pocket of pus, in an effort to contain the infection. Over time, the pressure within the abscess builds up. The body seeks the path of least resistance to drain this pus. Often, this means creating a tunnel that extends from the infected anal gland to the skin around the anus. That tunnel is the fistula. The abscess may be drained surgically, but if the underlying infected gland is not completely removed, the fistula persists.
Beyond perianal abscesses, other conditions and diseases can predispose an individual to fistula formation. Crohn’s disease is one of the most significant risk factors. This chronic inflammatory bowel disease causes deep, transmural inflammation of the intestinal wall, and fistulas are a well-known complication. In fact, up to half of all people with Crohn’s disease will develop a fistula at some point. Other inflammatory conditions, such as diverticulitis and ulcerative colitis, can also lead to fistula formation, though less commonly.
Infections like tuberculosis and sexually transmitted diseases such as lymphogranuloma venereum have been historically linked to fistulas. Trauma to the anorectal region, whether from childbirth (especially if a severe tear or episiotomy becomes infected), surgery, or foreign objects, can also initiate the process. Radiation therapy for pelvic cancers, such as cervical or prostate cancer, can damage healthy tissues and create an environment where fistulas can form years later. Lastly, certain lifestyle factors, including chronic constipation or prolonged diarrhea, increase the pressure and irritation in the anal area, potentially contributing to the blockage of anal glands.
The Multifaceted Effects of Living with a Fistula
The effects of a fistula extend far beyond physical pain. On a daily basis, the constant drainage and the need to manage cleanliness can be exhausting. Many individuals find themselves changing pads or undergarments multiple times a day, which disrupts work, social activities, and travel. The odor associated with the discharge is often a source of intense self-consciousness, leading people to avoid intimate relationships, public restrooms, and even close physical proximity with colleagues or friends.
Physically, untreated fistulas rarely heal on their own. Instead, they tend to follow a recurring pattern: the external opening closes temporarily, an abscess forms, the abscess bursts, and the cycle repeats. Over time, a single simple fistula can branch out, becoming a complex fistula with multiple tracts, which is much harder to treat. Furthermore, chronic inflammation and infection can weaken the anal sphincter muscles, the very muscles responsible for holding in stool. This can lead to fecal incontinence, a devastating complication where the individual loses partial or complete control over bowel movements.
Psychologically, the effects are profound. Depression, anxiety, and social withdrawal are extremely common among long-term fistula sufferers. The condition can feel shameful, and many people delay seeking medical help for months or even years because of embarrassment. This delay often allows the fistula to become more complicated, leading to poorer outcomes. Financial effects also pile up, as repeated doctor visits, medications, time off work, and potential surgeries create a significant burden.
Prevention: Is It Possible and How to Reduce Risk
Preventing a fistula is not always possible, especially when it arises from conditions like Crohn’s disease or after radiation therapy. However, the most common cause of anal fistulas, namely anal abscesses, can often be prevented through consistent and mindful habits. The cornerstone of prevention is avoiding the conditions that lead to anal gland blockage and infection.
The first and most important step is maintaining good anal hygiene. This does not mean aggressive scrubbing, which can cause micro-tears and irritation. Instead, gentle cleansing with warm water after each bowel movement, using a bidet or a soft, damp cloth, is ideal. Harsh soaps, scented wipes, and vigorous rubbing should be avoided. Keeping the area dry is equally essential, as moisture promotes bacterial growth. Wearing loose-fitting, breathable cotton underwear can help.
Diet plays a pivotal role. A diet rich in fiber from fruits, vegetables, whole grains, and legumes helps ensure soft, well-formed stools that pass easily without straining. Straining during bowel movements increases pressure in the anal region and can contribute to the blockage of anal glands. Drinking plenty of water, at least eight glasses a day, works alongside fiber to prevent constipation. Conversely, chronic diarrhea should also be evaluated and managed, as frequent loose stools can irritate the anal canal and increase infection risk.
For individuals with inflammatory bowel disease, strict adherence to medical treatment and regular monitoring by a gastroenterologist is the most effective preventive measure. Controlling the underlying inflammation dramatically reduces the likelihood of fistula formation. Additionally, anyone who notices symptoms of an anal abscess, such as a painful, swollen lump near the anus accompanied by fever or chills, should seek immediate medical attention. Early drainage of an abscess by a qualified professional, combined with appropriate antibiotics if necessary, can sometimes prevent the progression to a chronic fistula.
Homeopathic Remedies for Fistula: A Closer Look
Homeopathy offers a unique, constitutional approach to treating fistulas, focusing on the individual as a whole rather than just the local lesion. It is important to state clearly that homeopathy is not a substitute for emergency or surgical care, especially in the case of acute abscesses or severe infections. However, many patients seek homeopathic treatment either to manage chronic, non-healing fistulas, to prevent recurrence after surgery, or to address the underlying susceptibility that leads to repeated abscesses. Homeopathic remedies are selected based on the totality of symptoms, including the type of discharge, the nature of the pain, the patient’s temperament, and other unique characteristics.
Here are several homeopathic remedies that have been traditionally used in the management of fistulas, but they must always be prescribed by a qualified homeopathic practitioner after a thorough case-taking.
Silicea is often considered one of the most important remedies for fistulas that are slow to heal. It is indicated when there is a chronic, discharging fistula with thin, offensive, watery pus. The discharge may contain specks of blood. The individual often feels cold, is sensitive to drafts, and tends to have poor stamina. Silicea is known for its ability to expel foreign bodies and promote the healing of deep-seated, suppurating tissues.
Hepar Sulphuris Calcareum is another major remedy, particularly suited to fistulas that are extremely sensitive to touch and cold. The pain is often described as splinter-like, and the discharge is thick, yellow, and foul-smelling like old cheese. The person tends to be irritable and chilly. This remedy is especially useful when there is a tendency to form abscesses that do not mature easily or when the surrounding skin is easily infected.
Calcarea Sulphurica is a tissue salt that acts as a blood purifier and is indicated when the fistula drains a thick, yellow, or greenish-yellow pus. There may be recurrent abscesses in the same area. It is often used between acute flare-ups to help the body resolve chronic suppuration.
Myristica Sebifera, sometimes called the “homeopathic knife,” has a reputation for its ability to bring about resolution of abscesses and fistulas without the need for surgery. It is indicated for small, simple fistulas where there is a feeling of a foreign body and where suppuration is present. However, it is not a cure-all and works best when the constitutional picture matches.
For fistulas associated with hemorrhoids or a history of suppressed skin eruptions, Graphites may be considered. The discharge is typically sticky, honey-like, and thin. The skin around the anus may be raw, excoriated, and prone to eczema. These individuals often have a tendency to constipation with large, knotty stools.
It is vital to understand that homeopathy works by stimulating the body’s own healing response. Therefore, treatment can sometimes take weeks or months, especially for long-standing fistulas. A competent homeopath will also advise on diet, hygiene, and lifestyle changes alongside the remedy. In many cases, homeopathic treatment can be used before and after conventional surgical procedures like fistulotomy or seton placement to improve healing and reduce recurrence rates. However, complex or deep fistulas, especially those involving sphincter muscles, should never be managed by homeopathy alone without concurrent surgical evaluation.
Frequently Asked Questions About Homeopathic Remedies for Fistula
1. Can homeopathy completely cure a fistula without surgery?
This is the most common question, and the answer requires honesty. In a small number of simple, superficial, newly formed fistulas, especially those that have not yet developed multiple branching tracts, some homeopathic practitioners have reported complete healing with remedies like Silicea or Myristica Sebifera. However, for the majority of chronic, complex, or deep anal fistulas, homeopathy alone is unlikely to eliminate the physical tunnel structure. Where homeopathy truly shines is in managing recurrent abscesses, reducing the frequency and severity of flare-ups, promoting faster healing after conventional surgery, and addressing the underlying constitutional weakness that makes a person prone to fistulas in the first place. It is best used as a complementary approach alongside surgical consultation, not as a guaranteed replacement for the knife.
2. How long does it take for homeopathic remedies to show results in fistula cases?
Homeopathy works at the level of the body’s vital force, not as a quick symptom suppressor. Therefore, timelines vary greatly. In an acute setting, such as a painful abscess threatening to form a new fistula, a well-chosen remedy like Hepar Sulph or Belladonna may show improvement in drainage and pain reduction within 24 to 48 hours. For chronic, non-healing fistulas, however, patients typically need to take constitutional remedies for three to six months before noticing significant changes such as reduced discharge, less odor, and longer infection-free intervals. Patience is essential. If no improvement whatsoever is seen after four months of consistent homeopathic treatment under a qualified practitioner, it is wise to re-evaluate the approach.
3. Are there any side effects of using homeopathic remedies for fistula?
When prescribed correctly by a trained homeopath, these remedies are extremely safe, non-toxic, and free from the side effects associated with long-term antibiotic use or steroid therapy. Homeopathic medicines are prepared through potentization, which dilutes the original substance to minute levels. However, a phenomenon known as a “homeopathic aggravation” can sometimes occur, where symptoms temporarily worsen for a day or two before improvement begins. This is generally seen as a positive sign that the remedy is stimulating the body’s healing response. True adverse effects are exceptionally rare. That said, self-prescribing from internet lists without a constitutional evaluation can lead to ineffective treatment or suppression of symptoms, which is why professional guidance is strongly recommended.
4. Can I take homeopathic remedies along with my conventional medications or after surgery?
Absolutely. One of the great strengths of homeopathy is its ability to work harmoniously alongside conventional medicine. There are no known drug interactions between homeopathic remedies and antibiotics, painkillers, anti-inflammatory drugs, or even medications for Crohn’s disease. After a surgical procedure like a fistulotomy or seton placement, homeopathic remedies such as Staphysagria (for surgical wounds that are slow to heal with sharp, stitching pain) or Hypericum (for nerve-rich areas like the anal region) can significantly speed up recovery and reduce post-operative discomfort. Just be sure to inform both your surgeon and your homeopath about all treatments you are receiving.
5. How does a homeopath choose the right remedy for my fistula? Isn’t one remedy enough for everyone?
No, and this is a critical point. Homeopathy is not a one-size-fits-all system. Two people with anal fistulas may receive completely different remedies. For example, a person needing Silicea typically has a thin, watery, offensive discharge, feels cold and lacks stamina, and is mentally yielding. Another person needing Graphites may have a sticky, honey-like discharge, suffers from chronic constipation with large stools, and tends to be overweight with skin problems. A third needing Hepar Sulph is irritable, chilly, and experiences splinter-like pain at the slightest touch. The homeopath considers not just the fistula discharge, but your sleep patterns, food cravings or aversions, emotional state, thermal preferences (hot or cold), and your family medical history. This individualized approach is what makes homeopathy powerful.
6. Can homeopathy help with fistulas caused by Crohn’s disease?
Yes, and this is an area where homeopathy offers significant supportive value. Crohn’s disease is a constitutional autoimmune condition, and the fistula is a local manifestation of that systemic imbalance. A skilled homeopath will not just treat the fistula tract but will prescribe a deep-acting constitutional remedy based on your unique Crohn’s symptom picture. Remedies such as Merc Sol (for bloody, offensive stools with tenesmus), Arsenicum Album (for burning pain, anxiety, and exhaustion), or Sulphur (for chronic diarrhoea with redness and itching around the anus) may be indicated. While homeopathy cannot replace biologic drugs or immunosuppressants for severe Crohn’s, many patients find that adding homeopathic treatment reduces the frequency of fistula flare-ups and helps maintain remission.
7. Are there any dietary or lifestyle restrictions while taking homeopathic remedies for fistula?
Homeopathy does have some gentle guidelines to keep remedies working effectively. Strong substances like raw garlic, strong coffee, peppermint, camphor (found in many topical balms like Vicks VapoRub), and menthol are traditionally advised to be avoided within 15 to 30 minutes before and after taking the remedy, as their strong smells and chemical properties can potentially antidote the remedy’s energy. That said, sensible use of these substances throughout the rest of the day is usually fine. More importantly, dietary recommendations for fistula itself remain crucial: high fiber, plenty of water, soft stools, and avoiding spicy, oily, or excessively dry foods. Homeopathy works best when combined with good hygiene and proper nutrition.
8. How do I take homeopathic remedies correctly for fistula?
Homeopathic pills (usually lactose-based globules) are typically taken sublingually, meaning placed under the tongue and allowed to dissolve. Hands should be clean and dry, and you should avoid touching the pills directly if possible (use the cap of the vial). Do not eat, drink, smoke, or brush your teeth for at least 15 minutes before and after taking the remedy. The typical dosage for a chronic condition like fistula is a low potency (such as 6C or 30C) taken once or twice daily, or a higher potency (200C or 1M) taken less frequently, perhaps once a week or once a month under professional guidance. Never take a high potency repeatedly every day unless directed, as this can overstimulate and prove ineffective. Always follow your homeopath’s specific instructions.
9. Is homeopathy safe for fistulas during pregnancy or while breastfeeding?
Many homeopathic remedies are considered safe during pregnancy and breastfeeding because of their highly diluted nature, but this does not mean you should self-prescribe. Pregnancy alters the body’s immune response and hormonal balance, and a fistula that was stable may become more problematic. Remedies like Silicea and Calcarea Sulphurica are generally regarded as safe, but others such as Thuja or heavier metals should be avoided during pregnancy unless specifically indicated by an experienced homeopath who specializes in prenatal care. Always disclose your pregnancy status to your homeopath and obstetrician. In many cases, gentle local hygiene and dietary management may be recommended as the first line during pregnancy, reserving aggressive homeopathic treatment for the postpartum period.
10. How do I find a qualified homeopath for fistula treatment?
Not everyone who sells homeopathic pills or gives online advice is truly qualified. Look for a practitioner with credentials such as DHMS (Diploma in Homeopathic Medicine and Surgery), BHMS (Bachelor of Homeopathic Medicine and Surgery), or equivalent from a recognized institution. In countries like India, Germany, the UK, and parts of the US, there are regulatory bodies. A good homeopath will spend at least 45 to 90 minutes during your first consultation asking detailed questions about your physical symptoms, emotional state, sleep, digestion, temperature preferences, and life stresses. They should also ask about your surgical history and any conventional treatments you are undergoing. Be wary of anyone who prescribes a “fistula mixture” or the same remedy to every patient without a thorough case-taking. Reputable homeopaths will also know when to refer you back to a surgeon if the fistula becomes complex or infected beyond their scope.
Conclusion
A fistula is a challenging condition, but it is not a life sentence. Modern medicine offers effective surgical treatments with high success rates, and complementary approaches like homeopathy can provide valuable support. The key is early recognition of symptoms, prompt medical consultation, and a willingness to discuss the issue openly with a healthcare provider. No one should suffer in silence. By understanding the causes, recognizing the symptoms early, taking preventive measures, and exploring all available healing modalities responsibly, individuals can regain control over their health and their lives. Whether one chooses conventional surgery, homeopathic treatment, or an integrative approach, the path to healing begins with knowledge and the courage to seek help.